A solid understanding of the scientific foundation of anesthesia is essential for quality patient care and for achieving board certification. Therefore, the didactic aspect of our program is given a high priority.
Learning Opportunities
Rush Center for Clinical Skills and Simulation: provides individualized and group training simulation sessions focused on basic training and crisis management. Residents are assigned simulations throughout the year, as well as before the beginning of each specialty rotation that requires unique skills.
Image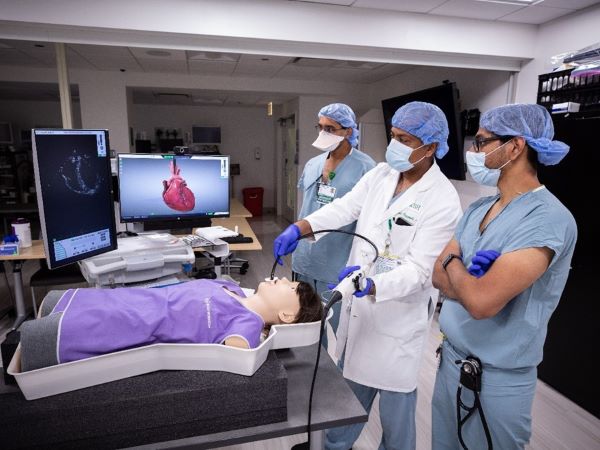
- Morning lectures: Morning lectures are given by faculty and focus on Basic and Advanced keywords as delineated by the America Board of Anesthesiology, as well as formal board review in a question/answer format. CA2s and CA3s attend conferences on Mondays and Fridays and CA1s attend conferences on Tuesdays and Thursdays.
- Curriculum based conferences are given by teaching staff on Monday evenings, 4 p.m. - 5 p.m.
- Grand rounds/visiting professor series are held on Wednesday mornings, 7 a.m. - 8 a.m.
- Clinical Excellence Conferences are held once per month on Wednesday, 7 a.m. – 8 a.m. to discuss notable cases with an updated literature review.
- Mock oral board exams are practiced throughout the year under the supervision of faculty members who are oral board examiners for the American Board of Anesthesiology (ABA). There are two Rush faculty members who are current ABA oral board examiners.
Journal club and dinner provided by the department quarterly, gives the residents and faculty members the opportunity to review and discuss journal articles in a collegial atmosphere. Articles are chosen with the intent to spark a lively discussion on the evolving state of anesthesia practice.
Image
- Specialized Seminars and Workshops:
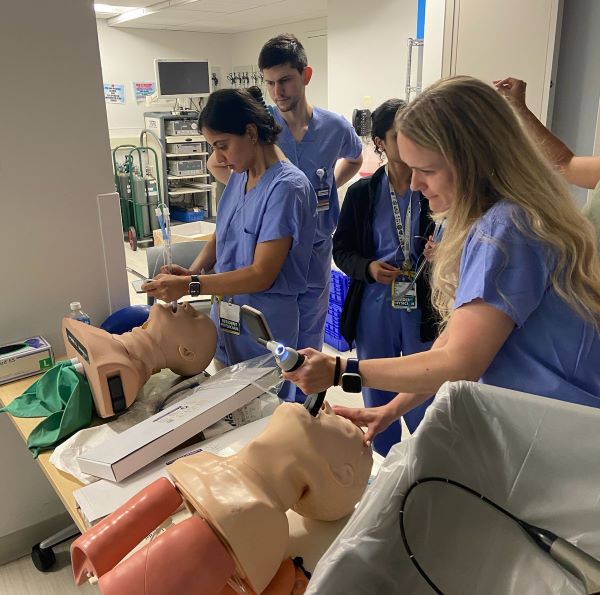
Difficult Airway Workshop: During the CA-1 year, all residents attend a well-structured training program in difficult airway management that includes fiberoptic intubation, supra-glottic airway device placement, double lumen and bronchial blocker placement, and advanced airway management. Residents have the opportunity to receive certification in fiberoptic intubation (FOI) after successful completion of 50 supervised procedures. Also, residents will receive training on performing surgical airways and retrograde intubations.
Regional Anesthesia Workshop: During the CA-1 year, the regional faculty members lead a regional workshop that includes an overview of the basic anatomy of the upper and lower extremities and hands on simulation of peripheral nerve blocks before residents begin their Regional 2 rotation.
Advanced Regional Anesthesia Workshop: During CA-2 year, the regional faculty members lead an advanced regional workshop that involves the use of ultrasound on standardized patients in the simulation center and a cadaver in the gross anatomy lab. These powerful educational tools help prepare CA-2 residents to perform numerous peripheral nerve blocks on patients.
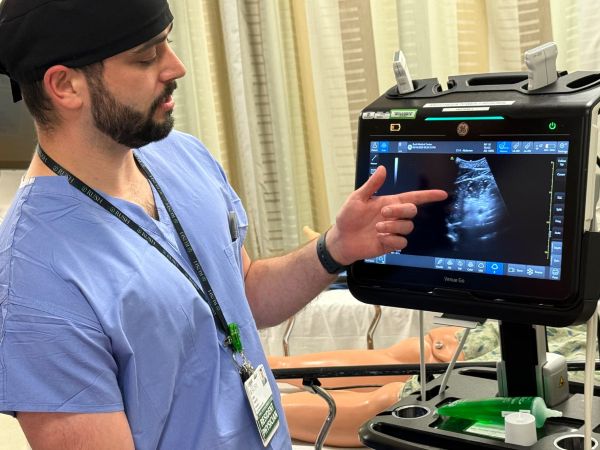
PoCUS Workshop: Faculty certified in Point-of-Care Ultrasonography (PoCUS) conduct workshops to train residents to perform transthoracic echocardiography as well as abdominal, lung, and gastric ultrasound exams.
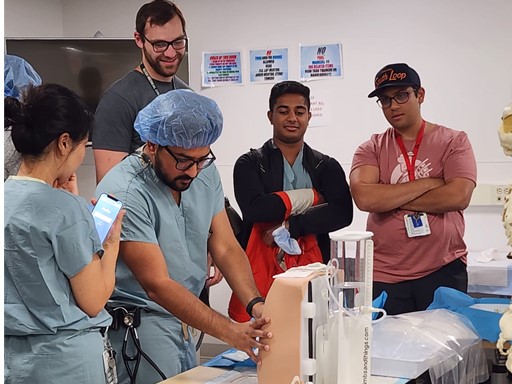
Transfusion Workshop: In these workshops, residents review the basics of blood product administration as well as how to deal with massive intraoperative blood loss. A key aspect of these sessions is individualized hands-on training on the set up of rapid transfusion devices.
CA3 Practice Management Seminar: We invite guest speakers to speak with our CA3 residents to discuss practice management, liability insurance and malpractice insurance. The purpose of the seminar is to provide as much information to our residents as they prepare for independent practice.

ASA Wood Library-Museum of Anesthesiology: While on their orientation month, CA-0 residents take a trip to the ASA Wood Library in Schaumburg, IL. The museum presents an interactive overview about the history of anesthesia. During the tour, they learn about important milestones throughout the timeline of the history anesthesiology.
Resources
Rush Library/Clinical Key: Residents have access to electronic versions of most anesthesia texts including Miller's Basics of Anesthesia, Miller's Anesthesia, Barash’s Clinical Anesthesia, and Stoelting's Anesthesia and Co-Existing Diseases.
TrueLearn: We provide residents access to TrueLearn during their clinical anesthesia years. TrueLearn provides anesthesia board questions specifically crafted by board-certified anesthesiologists to mirror those tested on ABA anesthesia exams.
ASA Anesthesia Toolbox: Residents have access to a collaborative project of over 60 academic programs to develop and share educational resources for anesthesia education. Multi-media peer-reviewed content, Wiki cases, and rotation curricula are some examples that ASA Anesthesia Toolbox has to offer.
Back to top
Resident Evaluation
- CA-0 residents are evaluated by the supervising attending physicians throughout each rotation. Residents’ performance and their education are closely monitored and evaluated by ACGME standards.
- CA-1, 2, and 3 residents:
- Each resident is evaluated by the supervising attending staff based on: 1) The level of patient care they provide 2) medical knowledge base 3) interpersonal communication skills 4) professionalism and ethics 5) practice-based learning and improvement 6) system-based practice in compliance with ACGME requirements. The evaluations become part of the resident’s permanent file, to which she/he has access.
- Periodically other members of the healthcare team, including nurses, resident peers, and a variety of support staff, are asked to complete a global (360 degree) evaluation of the resident.
- Yearly American Board of Anesthesiology (ABA) In-Training Exam (ITE)
- Participation in mock oral exams
- A formal review of all residents' performance takes place 2 times per year. A semiannual training and evaluation report are submitted to the ABA at the mid-point and end of each academic year.
Individualized simulation sessions in the Rush University Simulation Laboratory are videotaped and reviewed with each resident.
Back to top
Requirements for Completion
- Throughout the three years of clinical anesthesia training, the residents are required to maintain a score of 25th percentile or above for all ITEs.
- Residents are required to pass the Basic Anesthesia Exam.
- Residents are required to register for and take the USMLE Step 3/COMLEX-USA Level 3 exam by the end of their PGY2 year.
- Maintaining and updating an accurate ACGME case log and duty hour log is the responsibility of every resident.
