
The Department of Ophthalmology provides consulting, diagnostic and treatment services for all conditions affecting the eye. All subspecialties within Ophthalmology are represented by over forty highly respected faculty.
The Department of Ophthalmology at Rush provides patient care services in the following subspecialty areas:
-
Comprehensive OphthalmologyImage

Anjali S. Hawkins, MD, PhD
Assistant Professor and Director, Section of Comprehensive Ophthalmology
Image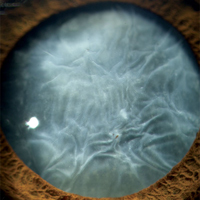
As a three resident-per-year program, one of the strongest aspects of ophthalmology training at Rush is the ability to learn comprehensive ophthalmology continuously for all three years. Residents follow their patients throughout their residency, developing a strong sense of continuity-of-care as a primary care doctor. State-of-the-art cataract extraction techniques are taught, including Femto-second laser assisted phaco, ORA aberrometer assisted surgery, and other modern image guidance technologies including the Callisto. The cataract surgery experience is quite busy, with most residents performing more than 200 procedures during their training. Residents benefit from having preoperative, operative, and postoperative contact with patients. The advantage of the rotational schedule, which allows continuity-of-care, ensures that patients who undergo surgery in the first or second year of training will be followed by the same resident for all three years. In general, routine procedures are performed during the first and second year, with more complicated operations and techniques being performed by the senior residents. Residents depart this program with the knowledge and expertise to be superb anterior segment surgeons. The Comprehensive Ophthalmology Section faculty who participate in the resident continuity clinic include Section Director Anjali S. Hawkins, MD, PhD, Thomas A. Deutsch, MD, Joseph B. Garber, MD, and Ronald S. Weiss, MD.
-
Cornea and External DiseaseImage
Vanee V. Virasch, MD
Professor and Director, Section of Cornea and External Disease
Image
The Cornea and External Disease Section is proud to have some of the country’s finest and most respected anterior segment specialists in the country. Corneal clinics are held multiple times a week to provide residents with the ability to closely follow cornea patients with acute pathology (corneal ulcers, inflammatory disease of the ocular surface, etc). By the end of the training period, residents are able to examine and treat patients with all aspects of corneal disease. Strong emphasis is placed on modern microbiologic evaluation and therapy. Residents gain experience in a variety of complex corneal surgical procedures, including combined keratoplasty/cataract extraction, penetrating and lamellar keratoplasty, temporary and permanent keratoprosthesis, keratoplasty associated with anterior chamber reconstructions and intraocular lens exchange with suture and intra-scleral haptic fixation of intraocular lenses. All of these procedures are often performed by the residents with faculty supervision. Strengthening the educational program are cornea journal clubs, case presentations, and didactic lectures supervised by the corneal attendings. The Cornea and External Disease Section faculty who participate in the resident continuity clinic include Section Director Vanee V. Virasch, MD, Sonya Bamba, MD, Rachel H. Epstein, MD, Parag A. Majmudar, MD. Jonathan B. Rubenstein, MD, and Anjali Tannan, MD, and Neel S. Vaidya, MD.
-
GlaucomaImage

Michael L. Savitt, MD
Assistant Professor and Director, Section of Glaucoma
Image
Specialty glaucoma clinics are held throughout the week so that complex glaucoma patients can be seen with fellowship trained glaucoma specialists. Additionally, glaucoma patients are seen in the general clinic with general ophthalmology attendings throughout the week. One resident reads
automated visual field tests one day per week in a one-on-one session. An excellent experience in surgical glaucoma therapy is provided; approximately four glaucoma surgical procedures are done each week, with residents as the primary surgeon in Eye Center cases. Surgical experience is gathered in standard trabeculectomy, MIGS procedures, antimetabolite assisted procedures, peripheral iridectomies, goniotomy, and placement of seton tubes and valves. Residents are expected to become proficient in all procedures as primary surgeon. In addition, experience is gained in cyclodestruction procedures with either cryotherapy, contact YAG or contact diode laser, selective laser trabeculoplasty, thermal laser trabeculoplasties and laser peripheral iridotomies. Emphasis is placed on modern nerve fiber analysis with the OCT. By the end of the training, residents are able to examine and treat all aspects of glaucoma medically and surgically. The Glaucoma Section faculty who participate in the resident continuity clinic include Section Director Michael L. Savitt, MD, MD, Madhu S.R. Gorla, MD, Nina A Goyal, MD, Anjali S. Hawkins, MD, PhD, Brian Herst, MD, Brian J. Jacobs, MD, Hreem Patel, MD, and Rebecca Sarran, MD. -
Neuro-ophthalmologyImage

Thomas R. Mizen, MD
Associate Professor and Director, Section of Neuro-ophthalmology
Image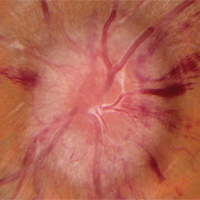
During the neuro-ophthalmology clinic, patients with a wide range of neuro-ophthalmologic problems are seen. Residents are expected to become proficient at complex neuro-ophthalmic examination, including visual fields, tangent screen, pupil analysis, MRI and CT scan, and CNS electrophysiology. Residents actively participate in surgical procedures, including orbitotomy, temporal artery biopsy, muscle surgery for cranial neuropathies and orbital thyroid disease, and they assist in optic nerve sheath fenestration. As neuro-ophthalmology is a cross-discipline field, residents learn the appropriate interaction with the related fields of neurology, neurosurgery, otolaryngology, oculoplastics, and radiology on a case-by-case basis. The educational program is enhanced by evening neuro-ophthalmic case conferences and journal clubs. At the completion of training, the residents are competent in the comprehensive evaluation of neuro-ophthalmological problems, both central and orbital, and perform complete neuro-ophthalmologic examinations. The Neuro-ophthalmology Section faculty includes Section Director Thomas R. Mizen, MD and Aimee J. Szewka, MD.
-
Ocular OncologyImage

Jack A. Cohen, MD
Associate Professor and Director, Section of Ocular Oncology
Image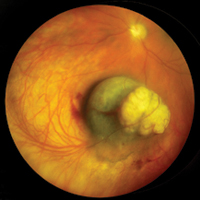
Rush residents have the unique opportunity to evaluate and manage patients who have benign and malignant tumors of the eye and adnexa. The ocular oncology service is under the direction of Jack A. Cohen, MD, the only fellowship trained ocular oncologist in Chicago. Each year, approximately 20 patients are seen with a variety of eye tumors. Dr. Cohen emphasizes preoperative, operative and postoperative management of these patients with the residents. Residents are exposed to the evaluation and follow-up of these patients, including standardized ultrasonography, radiology, MRI and CT scanning, and biomicroscopy. Additionally, experience with various surgical procedures is obtained, including fine needle biopsy, vitreous and conjunctival biopsy, plaque brachytherapy, external beam teletherapy, dosimetry, spray cryotherapy, transpupillary thermotherapy, chemoreduction and cryotherapy. Surgical therapy of orbital and adnexal tumors are coordinated with the Cornea and External Disease, Oculoplastic, and Neuro-Ophthalmology Sections. At the completion of training, residents are proficient in the recognition, management and referral of patients with a variety of ocular tumors.
-
Oculoplastics, Orbital, and Reconstructive SurgeryImage

Kenya M. Williams, MD
Assistant Professor and Director, Section of Oculoplastics, Orbital, and Reconstructive Surgery
Image
The Oculoplastic, Orbital, and Reconstructive Surgery Section provides an excellent balance of functional, reconstructive and cosmetic surgery throughout the residency. Residents participate as primary surgeon and assistant on a wide variety of surgical procedures, including ptosis and lid malposition repair, blepharoplasty, lid and orbital tumor removal and reconstruction, repair of orbital fractures and tear drainage abnormalities, repair of congenital abnormalities and surgical rehabilitation of the thyroid eye patient. As part of an interdisciplinary team, the Oculoplastic and Reconstructive Surgery Section works closely with the ENT, neurosurgical and the general plastics service to provide comprehensive facial reconstructive services. At the end of training, residents are able to perform a variety of basic plastic procedures seen in a comprehensive ophthalmic practice. The Oculoplastic, Orbital, and Reconstructive Section faculty who participate in the resident continuity clinic consists of Section Director Kenya M. Williams, MD, Tamara R. Fountain, MD, Krishna B. Patel, MD, and Kathryn P. Winkler, MD.
-
Ophthalmic PathologyImage

Richard J. Grostern, MD
Assistant Professor and Director, Section of Ophthalmic Pathology
Image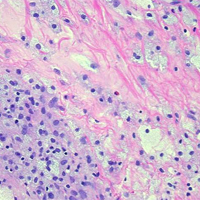
Richard J. Grostern, MD is fellowship trained in ocular pathology and oversee the department's clinical and educational pathology program. The resident laboratory experience takes place during the first year. Each first-year resident participates in two three-month rotations on the ophthalmic pathology service. Residents evaluate gross specimens and prepare them for fixation. Additionally, there are formalized one-on-one teaching with Dr. Grostern in the pathology lab. Although the volume of specimens derived from Rush patients is sufficient for the educational experience, additional unknown cases from the Ocular Pathology Library fortify the rotation. Dr. Grostern serve as ocular pathologist for the Cook County Medical Examiner. Emergency specimens can be processed and reviewed on virtually any day by the team. There is a one-hour block each month to conduct a pathology conference with the residents in morning didactic conferences.
-
Pediatric Ophthalmology and StrabismusImage

Diany S. Morlaes, MD
Assistant Professor and Director, Section of Pediatric Ophthalmology and Strabismus
Image
The pediatric clinic occurs weekly and pediatric patients are seen by all residents, especially by those in the first- and second-year. All residents may schedule strabismus operations with a pediatric specialist. Residents become proficient in amblyopia therapy, basic exotropia and esotropia surgery, and oblique dysfunction. The challenges of pediatric examination are taught by the experienced faculty, who all have busy pediatric private practices. Additionally, residents can participate in retinopathy of prematurity screenings and treatments in the neonatal intensive care unit, overseen by retinal specialist, Dr. Jack Cohen. By the end of the training period, residents are competent in examination and measurement of ocular deviations and the evaluation of all strabismus problems. The residents are also capable of making surgical decisions to engage in muscle surgery encountered in the average comprehensive practice. The Pediatric Ophthalmology & Strabismus Section faculty consists of Section Director Diany S. Morales, MD, Kimberlee Curnyn, MD, and Katherine Z. Brito, MD.
-
Refractive SurgeryImage

Jonathan B. Rubenstein, MD
Chairperson, Deutsch Family Endowed Professor and Director, Section of Refractive Surgery
Image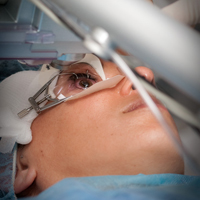
Rush is one of the few academic programs to have implemented a separate section of refractive surgery with a strong commitment and emphasis on resident education. The Eye Center has an on-site state-of-the-art wavefront guided excimer laser and femto-second laser. Second- and third-year residents rotate on the refractive surgery service and actively participate in the screening program, surgery and postoperative management. Residents are expected to become proficient in PRK and LASIK for a variety of myopic, hyperopic and astigmatic refractive errors. Complex cases due to keratoconus, and corneal thickness abnormalities are managed. Collagen corneal cross-linking is available to appropriate patient. Additionally, residents all gain experience in refractive cataract surgery and become comfortable using a variety of astigmatism and presbyopia correcting intraocular lenses throughout their third year of training. Morning refractive surgery rounds enhance the training. By the end of training, residents are able to implement refractive surgery into their practice. The Refractive Surgery Section faculty who participate in the resident continuity clinic include Section Director Jonathan B. Rubenstein, MD, Parag A. Majmudar, MD, Anjali Tannan, MD, and Vanee Virasch, MD.
-
Retina and Vitreous DiseaseImage

Vivek Chaturvedi, MD
Assistant Professor and Director, Section of Retina and Vitreous Disease
Image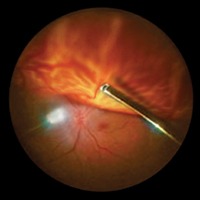
Rush is proud to have one of the most respected retinal programs in the Midwest. The resident retina clinics are held throughout the week. The residents are the first assistant or the primary surgeon in retinal and vitreous cases. Residents are exposed to all modern retinal surgical procedures, including 23 and 25 ga technology, 3-D heads up surgical microscopy, wide-field imaging, surgical adjuvants and tamponades, and a variety of surgical treatments for age-related macular degeneration. Throughout the three-year period, residents perform a high volume of laser and cryo procedures and intravitreal injections in the office, stressing treatments for diabetic retinopathy and macular degeneration. Enhancing the training experience, residents participate in retina journal clubs and monthly fluorescein and OCT conferences. By the end of the training period, each resident is competent in retinal examination and drawing, cryotherapy, panretinal photocoagulation, focal laser ablation of diabetes, and fluorescein angiography interpretation. The Retina and Vitreous Disease Section faculty who participate in the resident continuity clinic includes Section Director Vivek Chaturvedi, MD, Jack A. Cohen, MD, Sara Fard, MD, Henry Feng, MD, Ramon Lee, MD, Ryan Sabherwal, MD, and E. Anne Shepherd, MD.
-
Uveitis and Ocular InflammationImage

Veena Raiji, MD, MPH
Associate Professor and Director, Section of Uveitis and Ocular Inflammation
ImageUveitis patients are seen in the general clinics and during a specialty uveitis clinic on Friday mornings with Section Director Veena Raiji, MD, MPH. Residents become proficient in the complex workup of patients with uveitis, AIDS and immune disorders, including blood work, radiologic tissue typing, PCR testing of anterior and vitreous biopsy specimens, and retinal-choroidal biopsy. Residents learn the appropriate consultation needs with the rheumatology, infectious disease, and oncology services at Rush. In the training program, therapy with all levels of immune suppression and drug implant surgery are provided.
