
U.S. News & World Report’s 2024-2025 Best Graduate Schools rankings place the College of Nursing at No. 1 in Illinois – and five programs in the top three nationwide – while three College of Health Sciences programs earned strong rankings for quality.
Find information about application requirements, deadlines, and financial aid.

Find a list of College of Health Sciences programs with further information on individual program admissions.
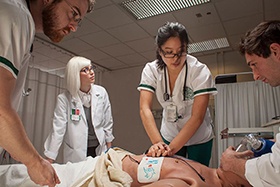
The College of Nursing uses a holistic admissions process. Learn about financial aid, grants and scholarships for students.

Find out more about the Graduate College’s list of requirements and necessary materials to submit via online application.

RUSH Medical College uses a holistic admission process to evaluate and select our class. Learn more about the process and RUSH Medical College.

Gain hands-on experience in clinical settings that provide high quality care and consistently rank among the best in the nation according to U.S. News and World Report.
According to the U.S. Department of Education, RUSH University leads Illinois universities in undergraduate students’ post-graduation earnings, with an average annual salary of $74,000.
Research awards have grown by 60% since 2019, and the 2021 total of $145 million in awards is a RUSH University record.
The College of Nursing's Faculty Practice delivers nursing services and direct care to diverse populations at more than 20 on sites across Chicago. One of these sites is a clinic at St. Leonard's Ministries. St. Leonard's provides formerly incarcerated men and women with housing, employment and educational services to help people transition back into the community. The Faculty Practice clinic manages health needs and fill gaps as St. Leonard's residents work toward establishing primary care providers for the time when they leave.
We host on-campus and online information sessions where you can learn more about specific programs. Click below to sign up for information on upcoming sessions in your program of interest.







