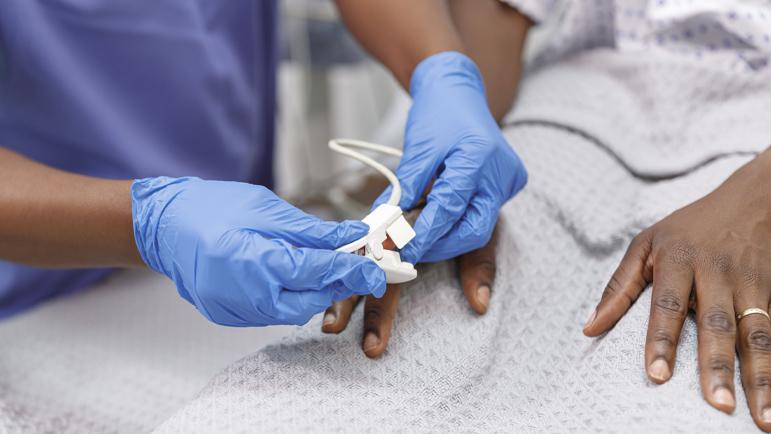
It’s a device most patients will recognize from their most recent doctor’s appointment: a small plastic clip attached to their finger that measures the levels of oxygen in their blood.
Called a pulse oximeter, it has become a critical diagnostic tool during the COVID-19 pandemic, with some patients even purchasing their own versions for home use.
But new research published in the Journal of the American Medical Association indicates that the oximeter is less accurate for patients with darker skin tones, and its inaccuracies may cause treatment for severe COVID-19 to be delayed or missed in patients of color.
“There’s been evidence for some time that pulse oximeters are not as accurate in persons with darker skin tones,” said Amanda Bradke, MD, an internal medicine physician at RUSH University Medical Center who co-authored the study. “We’ve reconfirmed that finding, and additionally showed this inaccuracy may have affected the way patients with COVID-19 were cared for.”
Inaccurate oxygen readings cause delayed COVID care
Researchers from RUSH, as well as from Johns Hopkins University and Baylor College of Medicine evaluated the medical records of patients with COVID-19 and found that pulse oximeters overestimated the blood oxygen levels in patients who identified as Black, Hispanic or Asian at a higher rate compared with white patients. Since the number on the oximeter was higher than the true number (confirmed with a blood test), this meant that their oxygen level was actually lower than the number being used to guide clinical care.
The oximeters also delayed showing eligibility for severe COVID-19 treatment more often in Black and Hispanic patients than in white patients. The oximeter is a key test used in determining whether patients are eligible for certain treatments for severe COVID-19.
“If your oxygen saturation is less than 94% on your pulse oximeter reading, that’s when most institutions would say you qualify for supplemental oxygen, dexamethasone, and remdesivir, among other treatments,” Bradke said. "These are treatments that that have shown improvement in morbidity and mortality in patients with severe COVID-19.”
A delay in the recognition for treatment eligibility occurred 29% more often in Black patients than in white patients, and in 23% percent more often in Hispanic patients than in white patients. There were also about 450 patients in the study where treatment eligibility was never recognized by the oximeter.
“The pulse oximeter never dropped below 94% throughout the study when it should have for these patients,” Bradke said. “Of those 450, just over half were Black.”
To conduct the study, researchers evaluated the records of more than 7,000 patients with COVID-19 from five referral centers and community hospitals in the Johns Hopkins Health System. They found 1,216 patients who had their blood oxygen levels measured with both the pulse oximeter and a more accurate blood test called an arterial blood gas (ABG) test within 10 minutes of each other and compared the two readings.
Why the device failed non-white patients
The pulse oximeter works by shining a light through the fingertip to analyze the oxygen content when the light passes through the finger. Bradke says that while the ABG test is more accurate, she
emphasized it cannot be used in all cases, as the blood test requires a specific needle stick in the wrist that not all medical personnel can easily do, as well as specialized analysis in a lab. Oximetry is non-invasive and can be used to monitor a patient continuously.
There has been a growing body of evidence showing that the oximeter is less accurate with darker skin tones since the 1990s. More recently, the Food and Drug Association released a safety communication in 2021, noting the evidence and providing guidance for patients on how best to use home oximeters.
Experts are still unsure exactly why the oximeter is less accurate in patients with darker skin tones, but they believe it may be because melanin, the substance that produces body pigmentation, absorbs more light. Research in this area has used race as a proxy for skin tone because information on skin tone wasn’t available.
“We do see this discrepancy for people who’ve identified as white as well, just not as often” Bradke said. “It might be something a little bit more nuanced, like if you have more yellow tones in your skin, or more red tones in your skin, that might be affecting the light rather than just the melanin. But we just don’t know.”
Identifying other areas where race impacts medical care
Bradke says the pulse oximeter is far from the only way that race is inappropriately addressed in medical testing and tools.
Bradke is co-director of the HEART (Health Equity and Anti-Racism Transforming Clinical Care) Committee at RUSH, which is working to evaluate medical decision tools that include race and eliminate those that perpetuate racism and exacerbate health care disparities. She does similar work in a coalition with other Chicago hospital systems called the Chicago Coalition for Anti-Racism and Equity (C-CARE) in Health.
The HEART Committee has already changed a kidney function test and pulmonary function test at RUSH that inappropriately used race in their equations, and recommended a heart medication for all patients that was previously only recommended for Black patients.
“When race is dealt with inappropriately in medicine it results in biased tools and tests,” Bradke said. “In the case of pulse oximetry, we think it’s because not enough people of varying skin tones were included in its development and validation, and an inequitable medical device was put into practice. It’s a problem with the device, whereas with other tools and tests, race was included where it shouldn’t be, as a biological risk factor to explain away the results of structural racism.”
A follow-up study is currently underway to determine if the delay in recognition of care eligibility led to changes in patient outcomes. Bradke said that patients and physicians should take care to look at the oximeter as just one piece of information in a patient’s larger clinical picture.
“It’s important to recognize that we’re using this imperfect tool in medical practice to help determine medical care,” Bradke said. “So it’s really important to pay attention to how you feel. It’s one piece of information, and if you’re not feeling well, if you’re walking across the floor and having a hard time breathing, but your oxygen says that you’re at 95%, maybe go in and get checked out anyways. And push to really look deeper into what’s going on.”